
Best Supplements for Pineal Gland Health: Ranked 1–10 by Evidence Score
10 pineal gland supplements ranked by evidence score — not marketing claims. Magnesium scored 8.4/10. Most popular products ranked lower...

Here’s the uncomfortable truth about pineal gland calcification: most adults already have it.
A 2023 systematic review published in Systematic Reviews (BioMed Central) found a pooled prevalence of 61.65% in the adult population. That’s not a fringe finding — that’s the majority of people reading this sentence. Which raises an obvious question: if calcification is that common, why does it matter? And if you’ve been wondering how to know if your pineal gland is calcified, the honest answer has two parts.
Part one: there are symptoms associated with calcification — sleep disruption, mood shifts, cognitive fog — backed by varying levels of evidence. Part two: none of those symptoms confirm calcification. The only thing that confirms it is medical imaging.
What follows is a breakdown of the 7 most reported signs, their actual evidence ratings, who’s at highest risk, and what a real diagnosis looks like. No mysticism. No invented studies. Just what we know, what we suspect, and where the research stops.
The pineal gland doesn’t calcify the way a pipe corrodes. It’s more deliberate than that — and stranger.
What happens: calcium phosphate crystals, known as corpora arenacea (or “brain sand”), accumulate within the glandular tissue over your lifetime. The process resembles bone formation mechanistically — involving mesenchymal stem cells and disruptions to calcium homeostasis within pinealocytes, as Tan et al. documented in their 2018 review in Molecules.
Why is the pineal gland so vulnerable? Because it sits outside the full protection of the blood-brain barrier. It’s a circumventricular organ — its capillaries are fenestrated, highly permeable, exposed to circulating minerals in ways most brain structures aren’t. A 2022 paper in Frontiers in Cellular Neuroscience confirmed this: the pineal receives some of the highest blood flow per gram of any tissue in the body, second only to the kidneys.
That’s a lot of circulatory exposure over a lifetime. It adds up.
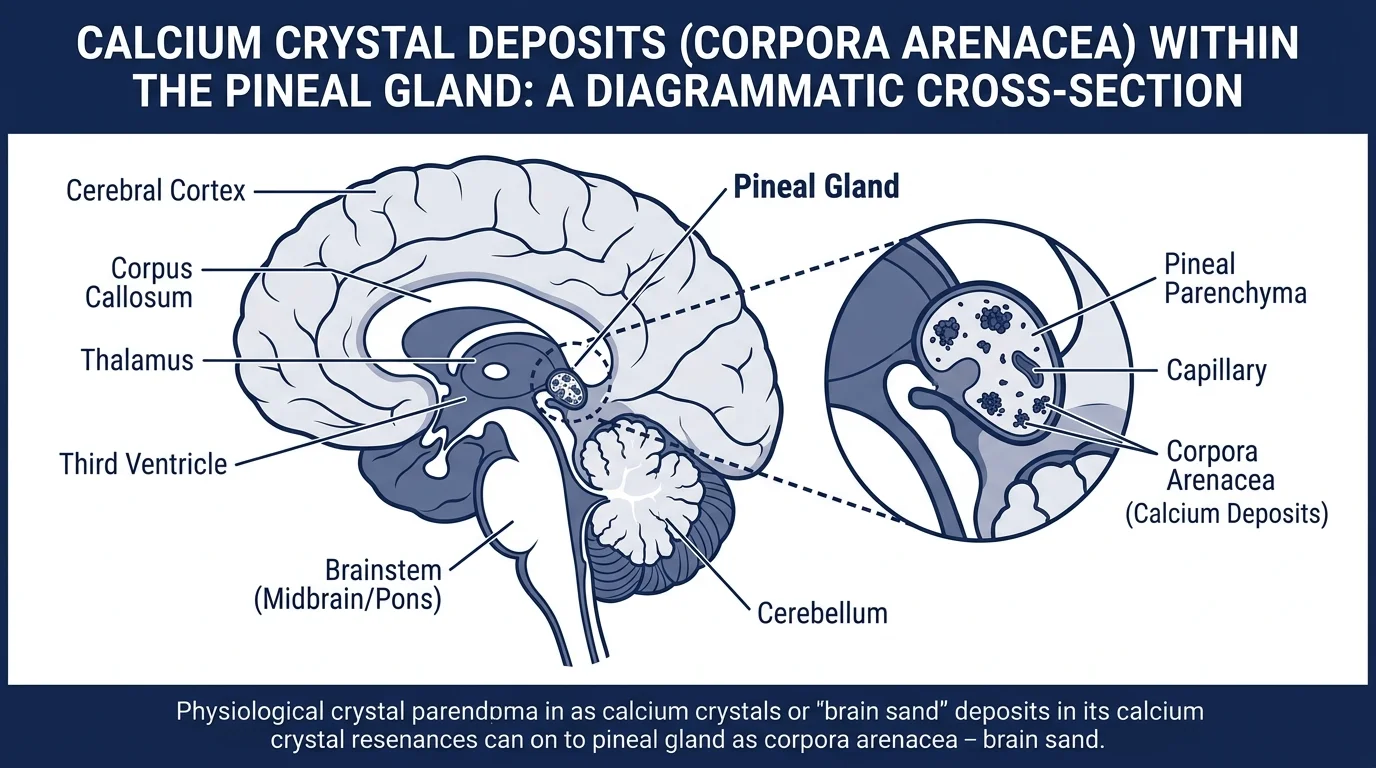
As calcification progresses, it compromises the gland’s ability to synthesize melatonin. A 1994 postmortem study in the Journal of Pineal Research found that age-related declines in melatonin biosynthesis may directly reflect altered calcium homeostasis in the pinealocyte. Radiologists have used pineal calcification as a midline landmark in skull X-rays for decades — which tells you how predictable and prevalent it is, even before modern neuroimaging.
For more on the downstream effects, see our overview of pineal gland calcification symptoms.
The most evidence-backed symptom is disrupted sleep — specifically insomnia and circadian dysregulation — linked directly to compromised melatonin output. Beyond that, the evidence gets thinner. Honesty requires saying that clearly.
Here are the 7 most reported signs, each rated by actual evidence quality.
Melatonin is the mechanism. The pineal gland is the primary source, and melatonin drives the sleep-wake cycle. When calcification reduces functional tissue, output drops.
A 1998 pilot study by Mahlberg et al. in Pathophysiology (n=36) found that greater degrees of pineal calcification correlated with chronic, subjective sleep-wake disturbances. Daytime fatigue was the primary reported symptom. Small study. No randomization. But the mechanism is physiologically sound — it’s the same mechanism explaining why melatonin production declines with age, tracking the same trajectory as calcification prevalence.
If your sleep has deteriorated without a clear lifestyle explanation and you’re over 30, this isn’t something to dismiss. For strategies specifically timed around sleep cycles, see pineal gland decalcification at night.
Both the Cleveland Clinic and Molecules (Tan et al., 2018) reference a loose link between pineal calcification and migraines — specifically, that reduced CSF melatonin levels may contribute to neurological vulnerability underlying cluster headaches.
The mechanism isn’t established. Association is not causation, and there are dozens of reasons someone develops chronic headaches. But melatonin has documented analgesic and anti-inflammatory properties in the CNS. A gland producing less of it is a plausible contributor.
Plausible isn’t proven. Worth noting, not worth diagnosing.
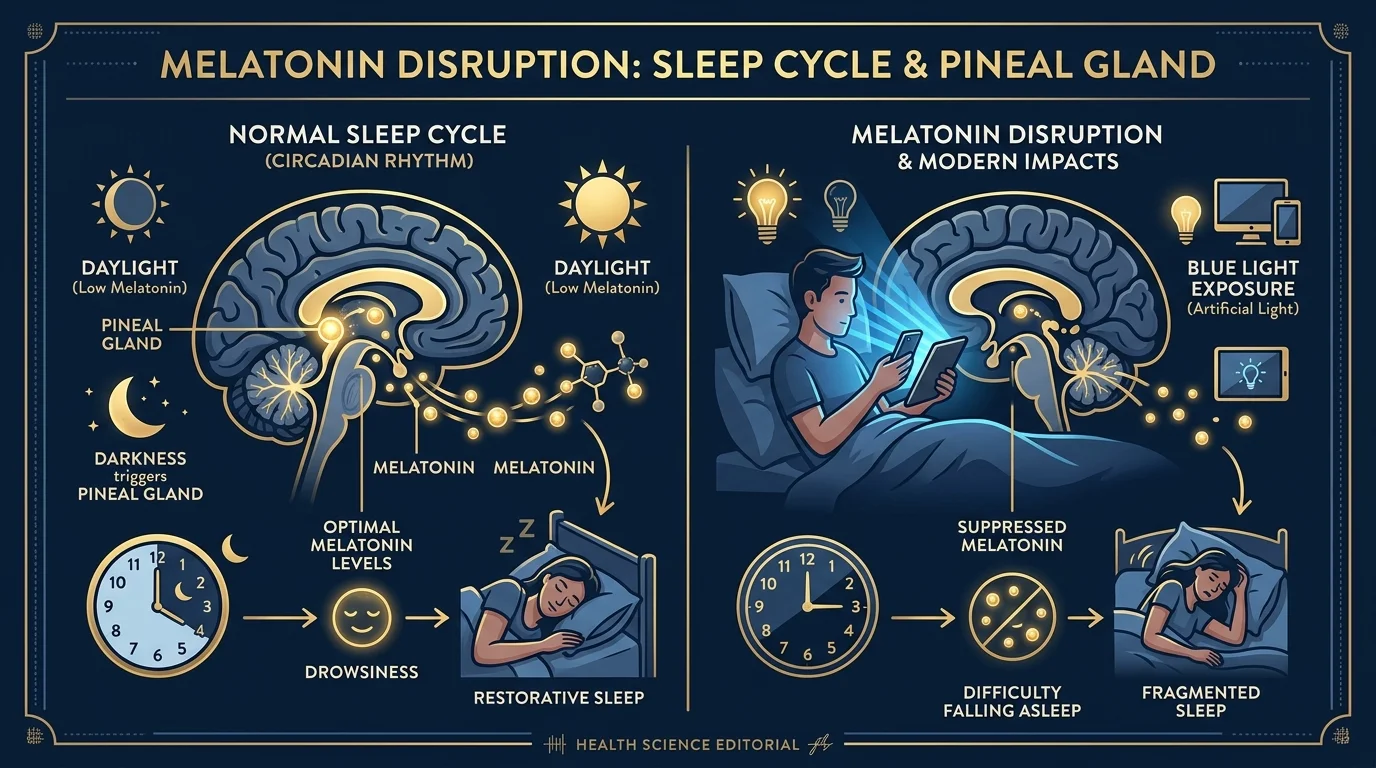
Melatonin doesn’t operate alone. It’s synthesized directly from serotonin, and disruptions in melatonin cycling have downstream effects on mood regulation. Calcification that impairs melatonin synthesis may influence the neurochemical balance underlying anxiety and mood stability.
The operative word: may. The studies are associative. Nobody has run a controlled trial showing that addressing pineal calcification improves anxiety outcomes. What exists is a biologically plausible pathway and population-level correlations. That’s enough to take seriously — not enough to take as gospel.
This is where the Alzheimer’s research becomes relevant — and where precision matters most.
A 2006 study by Mahlberg et al. in Neurobiology of Aging examined 279 patients at a memory clinic. Alzheimer’s patients showed significantly less uncalcified pineal tissue (mean: 0.15 cm²) compared to controls (0.25 cm²; p=0.027). A 2019 review in Current Alzheimer Research (Bhowmick et al.) documented that progressive pineal calcification in AD patients tracks with cognitive decline and sleep disruption.
Here’s what the data doesn’t say: that calcification causes cognitive decline. Both calcification and neurodegeneration accelerate with age. In some individuals, they accelerate together. “Associated with” and “causes” are not interchangeable. That distinction matters a lot, and most articles in this space don’t make it.
If sign #1 is about sleep quantity, this is about sleep architecture. Without adequate melatonin signaling, the circadian clock loses its primary chemical anchor — falling asleep at wrong times, waking at 3am fully alert, groggy until noon regardless of how long you were horizontal.
The physiology is textbook. What’s less clear is the degree to which calcification specifically — rather than age-related melatonin decline from all causes — explains it in any given individual.
Downstream from signs #1 and #5. If pineal output is compromised, you may log 7–8 hours and still wake unrested — because the melatonin cycle governing sleep depth and REM architecture has been disrupted upstream.
The Mahlberg pilot study flagged daytime fatigue as the primary symptom in patients with higher calcification grades. Small study. Associative design. No causal claim. But the pattern fits the mechanism.
This shows up frequently in forums and alternative health spaces. The logic isn’t absurd — the pineal gland receives photic input through the retinohypothalamic tract, and a compromised gland might theoretically alter that sensitivity.
No controlled studies link light sensitivity to pineal calcification as an isolated variable. It lives in anecdotal reports. That’s why it gets the red badge. I’m listing it because people report it consistently enough to acknowledge. I’m rating it red because honest is more useful than hopeful.

Calcification rarely appears before age 10 — prevalence sits around 1.1–4.2% in early childhood. By age 18, that climbs to roughly 33%, according to a 1987 radiographic study in Rofo. The 2023 meta-analysis by Belay and Worku puts pooled adult prevalence above 61%.
The process accelerates through adolescence and early adulthood, plateauing around age 30. You don’t “develop” calcification in old age. You carry it forward from much earlier — which is the part nobody mentions.
The pineal gland accumulates fluoride. That’s not speculation — it’s documented in a 2001 study by Jennifer Luke published in Caries Research. Postmortem analysis found mean fluoride concentrations of 297 mg F/kg of wet pineal tissue. Higher than bone. The correlation between fluoride concentration and calcium in the gland was statistically significant (r=0.73; p<0.02).
Important limitations: n=11 cadavers, no functional data from living individuals, high inter-individual variability. But the finding has never been formally disputed in the peer-reviewed literature, and that says something. For the full picture, we cover all the fluoride data here.
Additional factors in the literature: obesity, low-altitude environments, limited sun exposure, and potentially high EMF exposure — though the EMF data is considerably softer. An antioxidant-rich diet has appeared in preliminary research as potentially protective against oxidative stress in the gland — for a breakdown of specific foods with evidence behind them, see pineal gland foods.
The 2023 meta-analysis flagged male sex and white ethnicity as correlating with higher calcification prevalence in qualitative analyses. Effect sizes weren’t dramatic, and the authors were cautious about confounders. Still a pattern that appears consistently enough to note.
Here’s what nobody says clearly enough: you cannot self-diagnose pineal gland calcification. The symptoms above are non-specific. Poor sleep, brain fog, mood shifts — that describes roughly 40% of adults for dozens of reasons that have nothing to do with the pineal gland.
Symptoms are a reason to investigate. They are not a diagnosis.
The confirmed methods:
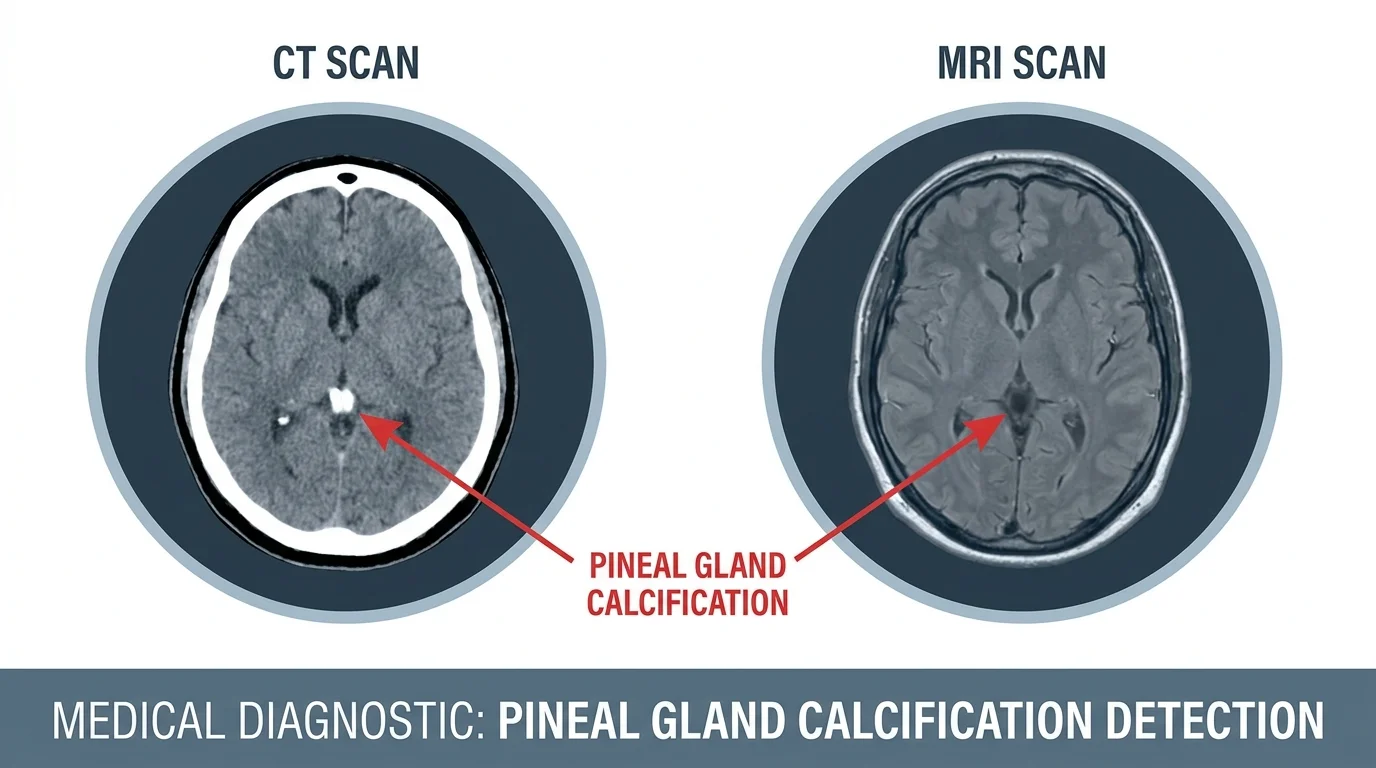
CT scan is the gold standard. Calcification shows up in the vast majority of adults on a standard cranial CT, often found incidentally — radiologists have used it as an anatomical landmark for decades precisely because it appears so consistently.
MRI with susceptibility-weighted imaging (SWI) is the most accurate alternative. A 2017 study in European Radiology (Seeger et al., n=384) found SWI reached 95% sensitivity and 96% specificity for pineal calcification detection — against 43% sensitivity for conventional MRI. No ionizing radiation, high accuracy. That gap is significant.
Lateral skull X-ray detects calcification in roughly 50–70% of adults. Lower sensitivity, but historically standard before CT.
Serum melatonin testing doesn’t confirm calcification. It can indicate functional impairment — but calcification grade and melatonin output don’t map onto each other linearly. How much functional tissue remains varies widely between individuals.
If you have persistent, unexplained sleep disturbance or cognitive changes you can’t account for, talk to a neurologist. Not a supplement stack. A neurologist.
What we know: pineal calcification is common, measurable, and mechanistically tied to melatonin decline. What we don’t know: whether any specific intervention meaningfully reverses it in living humans. No randomized controlled trial has shown that. The research isn’t there yet.
That doesn’t mean nothing helps.
Reducing fluoride exposure (filtered water, fluoride-free toothpaste), prioritizing antioxidant-rich foods, protecting sleep hygiene, managing light exposure after dark — these are evidence-adjacent strategies that support the melatonin system regardless of calcification status. Not cures. Levers.
For a structured approach to the reversal question, see how to reverse pineal gland calcification.
If you’ve already done the foundational work and want a targeted supplement, Pineal XT is one of the few formulations in this space built around the pineal gland’s documented biology — not vague “third eye” positioning. It won’t undo decades of calcification overnight. Nothing will. But if you want to support the gland running your melatonin production, it’s worth a look.
Quick Verdict — Pineal XT

Formulated around the pineal gland's documented biology — iodine for fluoride displacement, plus antioxidant compounds targeting the gland's high oxidative exposure. Lower price point than most competitors in this category. A reasonable option for those looking to support melatonin production at the source.

Marcus Hale is an independent researcher and former clinical neuroscientist. The content on PinealCode.com is for informational purposes only and does not constitute medical advice.

10 pineal gland supplements ranked by evidence score — not marketing claims. Magnesium scored 8.4/10. Most popular products ranked lower...
One peer-reviewed study found 9,000 ppm of fluoride in human pineal glands — 18,000x more than in muscle. Here's what that data means, what...
61.65% of adults have pineal calcification — and the internet promises a 30-day fix. Actual research timeline: 3–6 months. Week-by-week...

Marcus Hale
Independent Researcher · Former Clinical Neuroscientist
I spent 12 years in clinical neurology before the questions got more interesting than the answers. PinealCode is where I document what I find at the intersection of brain science and consciousness.