How Long to Decalcify Your Pineal Gland? Not 30 Days
61.65% of adults have pineal calcification — and the internet promises a 30-day fix. Actual research timeline: 3–6 months. Week-by-week...
Here’s what bothers me about this conversation: fluoride accumulates in your pineal gland. That’s not conspiracy. That’s in the peer-reviewed literature. The 2001 study by Jennifer Luke at the University of Surrey found an average concentration of 297 mg F/kg in the pineal gland—higher than in any other soft tissue in the body. Some samples went to 21,800 mg/kg.
But here’s where it gets complicated. And it’s complicated in a way that matters.
The presence of fluoride in the pineal gland doesn’t automatically mean dysfunction in living humans. We don’t have that data. And the absence of data isn’t the same as proof of safety. This is the gap where most people either panic or dismiss the whole thing. Neither response is rational. Neither is useful.
What follows is what the actual research shows, what remains unknown, and what you can reasonably do about it. No mythology. No false certainty.

Yes — but the story is more complicated than most sources admit. Fluoride accumulates in the pineal gland at concentrations higher than in any other soft tissue in the body. The 2001 study by Jennifer Luke at the University of Surrey found an average of 297 mg F/kg, with a correlation of r=0.73 between fluoride and calcium content — peer-reviewed and published in the Journal of Pineal Research.
What’s NOT documented: functional impairment in living humans at typical exposure levels. The distinction between “fluoride accumulates there” and “fluoride is damaging your pineal gland” is where most internet content goes wrong — in both directions.
Fluoride is a biological accumulator. It’s attracted to calcium. The pineal gland mineralizes with age—it accumulates calcium phosphate, and increasingly, fluoride binds to those minerals. This isn’t controversial. The mechanism is well-established.
Luke’s 2001 analysis is still the gold standard. Eleven cadavers, ages 50-92. The correlation between fluoride concentration and calcium content in the pineal gland was significant: r=0.73, p<0.02. That’s not weak. But—and this is critical—the study examined tissue from deceased individuals. It tells us about accumulation. It tells us nothing about functional impact in living brains.
The animal research goes further. In a 1997 study, Luke found that fluoride in gerbils inhibited melatonin synthesis and accelerated sexual maturation. Melatonin is what your pineal gland produces. It regulates sleep, immune function, and circadian rhythms. If fluoride impairs this in living humans, that matters — and the symptom picture of impaired melatonin production is documented in the pineal gland calcification symptoms guide.
But it’s gerbils.
The translational leap from rodent neurobiology to human neurochemistry is massive. Gerbils metabolize fluoride differently than humans. They don’t drink fluoridated water at 0.7 mg/L for seventy years—the exposure profile is completely different. The doses in the animal studies were often higher than typical human exposure. This doesn’t mean the findings are irrelevant. It means they’re not proof.
A 2016 analysis by Johns and Subongkot examined forty-two cadavers and found something interesting: the correlation between fluoride and pineal calcification was significant only above 50 mg F/kg. Below that threshold, there was no clear relationship. Most people in fluoridated areas don’t reach those levels. Most.
The pineal gland has unique vascularization—it’s highly perfused, meaning blood flows through it aggressively. Fluoride, once absorbed into the bloodstream, travels readily to mineralized tissues. The pineal gland, as it ages, mineralizes. Calcium, phosphate, and increasingly, fluoride, deposit there. It’s not a conspiracy. It’s biochemistry.
Strong enough to measure. Not strong enough to predict individual outcomes. That’s the honest answer.
This is where the conversation usually stops in mainstream health discourse. And that’s exactly where the real questions begin.
Here’s the single most important statement in this entire article: To our knowledge, there are no studies in living humans on the direct effects of fluoride exposure on the pineal gland or melatonin production. That quote comes directly from the 2021 Canadian environmental health study. Let it land. We’ve measured fluoride in cadaver tissue. We’ve seen effects in animals. We have zero direct measurements of melatonin suppression in living humans exposed to fluoride.
Zero.
What we do have are indirect associations. The 2021 Canadian study found that fluoride exposure correlated with shorter sleep duration in adolescents and adults. The hypothesis? Calcified pineal gland, reduced melatonin production, disrupted circadian rhythms. It’s plausible. It’s not proven. The study measured fluoride and sleep—not fluoride, pineal function, and sleep.
But there’s more data on neurodevelopment, and it matters for this conversation.
The National Toxicology Program completed a systematic review in 2024 on fluoride and neurodevelopment. Eighteen of nineteen high-quality studies showed an inverse association between fluoride exposure and IQ in children. The effect size was moderate. The exposure levels, however—this is crucial—were almost exclusively above 1.5 mg/L. The United States standard is 0.7 mg/L. Much of the evidence comes from countries with naturally elevated fluoride: Iran, India, China, areas where fluoride concentration is two to three times higher than what most Americans encounter.
Then in January 2025, a meta-analysis in JAMA Pediatrics synthesized seventy studies on fluoride and IQ. The association held. The caveat remained: most studies examined populations with high exposure, not typical U.S. fluoridation levels.
The EPA announced a review of its fluoride standard in April 2025. After forty years, they’re reconsidering. That’s not proof of danger. That’s institutional acknowledgment that the data merits re-examination.
Fluoride exposure is everywhere. Your water. Your toothpaste. Tea. Processed foods. You can’t randomize people into high-fluoride and no-fluoride groups for decades to see what happens. So researchers work with population-level data, dietary recall, and biomarkers like urinary fluoride. All useful. None definitive.
The gerbil data is compelling because the mechanism is clear: fluoride suppressed melatonin synthesis at the molecular level. But gerbil pineal glands aren’t human pineal glands. Their circadian biology isn’t identical. Their cumulative exposure profiles are different. The fact that something happens in an animal model doesn’t tell you it happens in you, at your dose, over your lifetime.
This isn’t dismissing animal research. It’s being honest about its limits.
The internet will tell you two incompatible things. One: fluoride is a mind-control agent, the pineal gland is your third eye, and water fluoridation is a government plot. Two: fluoride is completely harmless, calcification in the pineal gland is irrelevant, and anyone questioning this is delusional.
Both camps are wrong.
The first has no credible mechanism and zero evidence of intentional harm through fluoridation policy. It conflates a real phenomenon—fluoride accumulates in the pineal gland—with a fantasy about control. The second ignores the actual data: fluoride does accumulate, it does correlate with calcium content, it may affect melatonin production in some contexts, and the research in humans is genuinely incomplete.
The rational position lives in a third place: fluoride accumulates in the pineal gland; we don’t know the functional significance in living humans at typical exposure levels; precaution is reasonable. If you’re interested in what actually does move the needle for pineal function, the evidence points toward practices covered in how to open your third eye — meditation, light exposure, and breathwork have far more research behind them than any detox protocol.
And precaution doesn’t require panic.
The EPA is reviewing standards. Legitimate institutions are revisiting the evidence. This isn’t conspiracy—it’s how science actually works when questions are unresolved. The conversation is open because the data is incomplete. That’s not a reason to fear. It’s a reason to act thoughtfully.
Most Americans (72.3% according to CDC data from 2022) drink fluoridated water, typically at 0.7 mg/L. That’s the Public Health Service standard, set in 1986. The EPA’s maximum contaminant level is 4.0 mg/L, a ceiling set to prevent dental fluorosis, not based on pineal gland health.
Your actual exposure is broader than water alone.
Toothpaste is often the largest source of fluoride for children, especially if they swallow it. Adults absorb fluoride from toothpaste too, though in smaller quantities. Black tea contains naturally occurring fluoride, often in the range of 0.5-2.0 mg/L. Some varieties go higher. Grape juice, processed with fluoridated water, carries fluoride. Medications sometimes do. Infant formula mixed with fluoridated water.
Here’s how to think about it: total exposure matters more than any single source. If you drink fluoridated water (0.7 mg/L), brush with fluoride toothpaste twice daily, and drink black tea, you’re probably in the range of 1.0-1.5 mg/L total daily intake. That’s still below the levels where animal studies show effects. It’s not zero risk. It’s manageable risk.
The question becomes: do you want to reduce it?
If your answer is yes, read our full decalcification guide for a comprehensive protocol. This section covers the actionable stuff right now.
Start with water filtration. Reverse osmosis systems remove 90-95% of fluoride. Activated alumina filters also work—they’re cheaper, less waste, though slightly less effective. If you have the budget, invest in the reverse osmosis system. This eliminates your largest single exposure source.

Switch to a non-fluoride toothpaste. Hydroxyapatite-based options—brands like Boka or RiseWell—use the same mineral that comprises tooth enamel. The research on hydroxyapatite’s effectiveness at preventing cavities is solid. You’re not sacrificing dental health.

Reconsider black tea consumption, or at least rotate it out. Green tea contains less fluoride. Herbal teas contain almost none. This isn’t about complete elimination—it’s about distributing your sources so no single one dominates.
Dietary support matters. Minerals that compete with fluoride for absorption and excretion include magnesium, boron, iodine, and vitamin K2—and for a comprehensive supplement comparison for fluoride displacement, the evidence for each compound is mapped against clinical thresholds. A 2002 study by Bhattacharya found that tamarind increased urinary fluoride excretion by 91% in children. The mechanism involves tartaric acid binding to fluoride. You can get tamarind paste at most Asian markets. Use it as a condiment or in water.
Increase dietary iodine. Fluoride and iodine compete for thyroid uptake—adequate iodine may reduce fluoride absorption. Add seaweed snacks, iodized salt, or a modest iodine supplement (100-200 mcg daily) if you’re not getting it from food.
Magnesium is central to pineal function. The gland requires it for melatonin synthesis. Most Americans are deficient. Leafy greens, seeds, nuts, and high-quality supplements (magnesium glycinate absorbs best) support both pineal health and fluoride excretion.
Vitamin K2 directs calcium to proper tissues—bones and teeth—and away from soft tissue calcification. Natto, aged cheeses, and K2 supplements (if you can’t tolerate the food sources) address this directly.
Boron appears in the research as a mild fluoride antagonist. Brazil nuts, avocados, and chickpeas contain meaningful amounts. A standard intake of these foods provides adequate boron without supplementation.


If you’re doing everything above and want additional support, Pineal Guardian combines these minerals and bioactive compounds in a single protocol. It’s positioned as foundational support within a broader strategy of precaution—not as a cure or treatment, but as nutritional insurance while you’re filtering your water and adjusting your diet.
Most people feel the shift within 4-6 weeks: clearer sleep, sharper morning clarity. It’s not melatonin. It’s not a drug. It’s giving your body the minerals it actually needs to function while reducing fluoride exposure.
Fluoride accumulates in the pineal gland. That’s a fact. Whether this produces measurable dysfunction in you, at your exposure level, over your lifetime—that’s genuinely unknown. The research in living humans doesn’t exist yet.
But the precaution required to reduce fluoride exposure is minimal. It’s not expensive. It doesn’t require lifestyle contortion. Filtering your water, switching toothpaste, and supporting your mineral status with better nutrition—these are moves that benefit you regardless of the fluoride question.
They improve sleep. They support cognitive function. They’re smart moves on their own merits.
If you want to move on this today, start with your water filter. That’s the leverage point. Then read our full decalcification guide for the complete protocol. And if you decide to support this with supplementation, Pineal Guardian is designed specifically for this context — I’ve reviewed the full formula and ingredient evidence in the Pineal Guardian review.
The science is incomplete. Your agency isn’t.
Marcus Hale is an independent researcher and former clinical neuroscientist. The content on PinealCode.com is for informational purposes only and does not constitute medical advice.

61.65% of adults have pineal calcification — and the internet promises a 30-day fix. Actual research timeline: 3–6 months. Week-by-week...
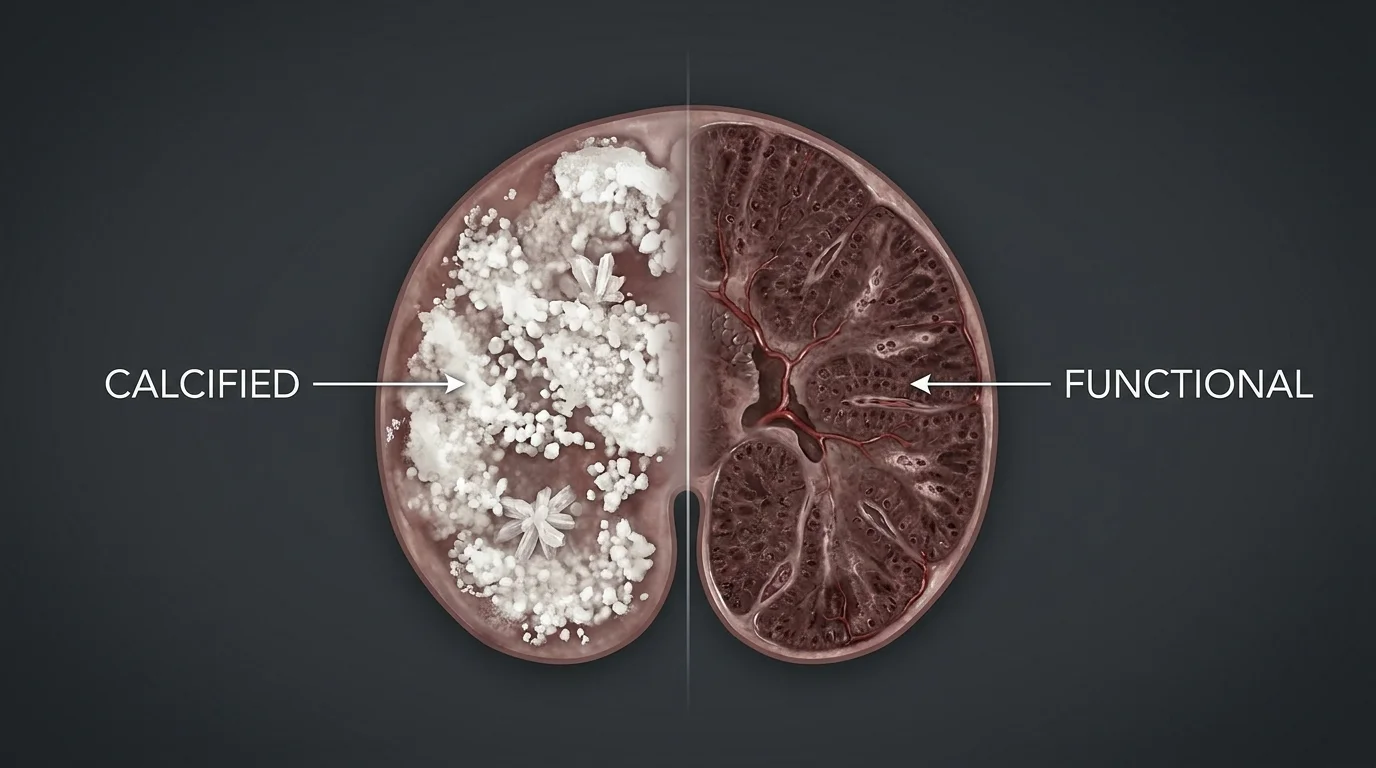
Can pineal gland calcification be reversed? Yes — with important caveats. See what the research shows, what works, and realistic timelines.
Only 5 ingredients pass the evidence check for pineal detox. Tamarind reduced fluoride 37% in a human trial. Here's the real protocol — and...

Marcus Hale
Independent Researcher · Former Clinical Neuroscientist
I spent 12 years in clinical neurology before the questions got more interesting than the answers. PinealCode is where I document what I find at the intersection of brain science and consciousness.