
Best Supplements for Pineal Gland Health: Ranked 1–10 by Evidence Score
10 pineal gland supplements ranked by evidence score — not marketing claims. Magnesium scored 8.4/10. Most popular products ranked lower...
Everyone in this space acts like the fluoride-pineal story is either completely proven or completely fabricated. Neither camp is right.
There’s one legitimate peer-reviewed study showing fluoride accumulates in the human pineal gland at concentrations that should, at minimum, make researchers uncomfortable. There are animal studies suggesting functional consequences. And there’s a gap the size of a canyon — no human clinical trials, no longitudinal data, no dose-response curve in living people — that both sides conveniently ignore when it suits them.
I spent 12 years in clinical neuroscience. I know how to read a methods section. The fluoride pineal gland calcification question deserves a real answer, not a dismissal dressed as skepticism. If you want the broader picture on how fluoride interacts with pineal gland biology, we’ve covered that separately. Here, we’re focused on the calcification claim specifically — what the data says, and where it stops.

The research here begins and more or less ends with one person: Jennifer Luke, a researcher at the University of Surrey who in 1997 completed a PhD dissertation on fluoride’s effects on pineal physiology, then published the key findings in Caries Research in 2001.
Here’s what she found.
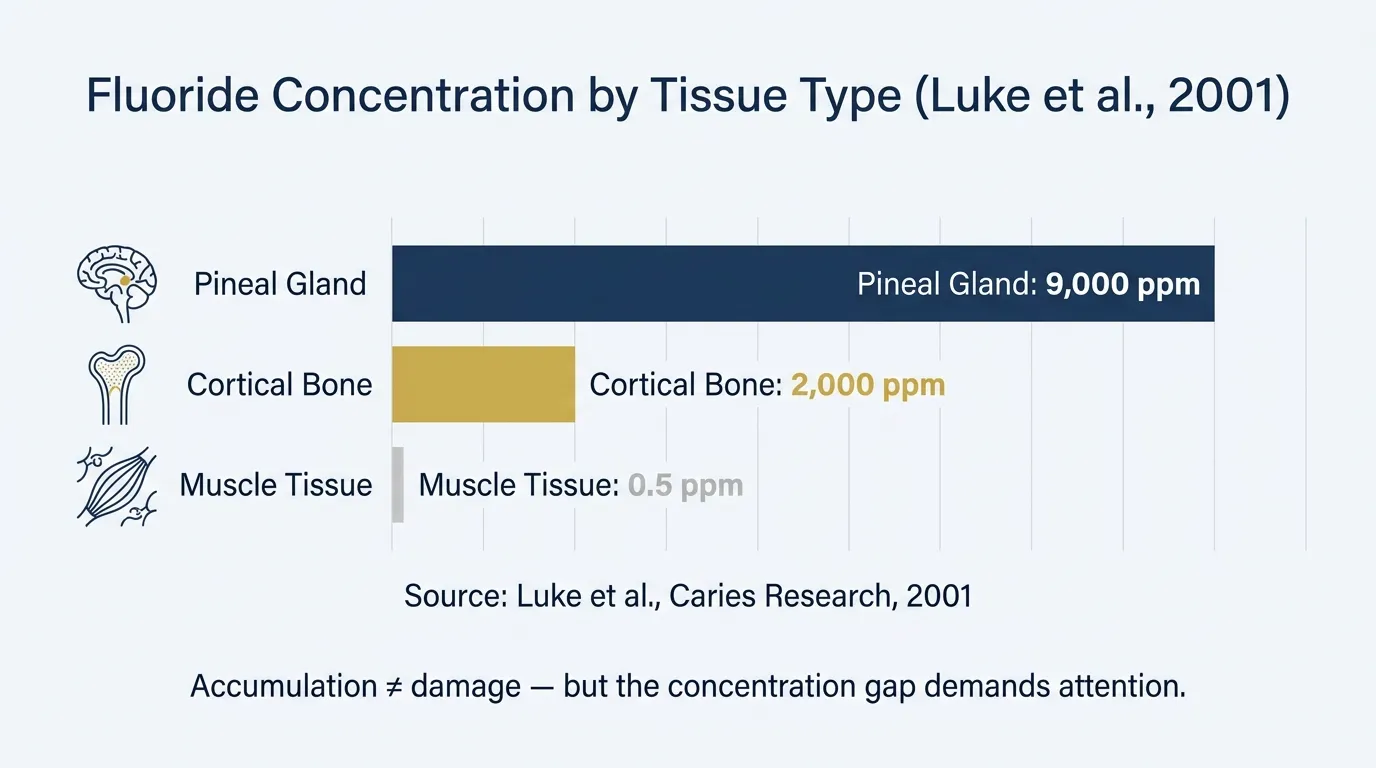
Luke dissected pineal glands from 11 aged human cadavers and measured fluoride concentrations. The average: approximately 9,000 parts per million in the pineal tissue. Muscle tissue from the same cadavers? About 0.5 ppm. Cortical bone? Around 2,000 ppm.
Fluoride accumulates in the human pineal gland at concentrations averaging 9,000 ppm — higher than in cortical bone (~2,000 ppm) and dramatically higher than in surrounding muscle tissue (~0.5 ppm), according to Luke et al. (2001) published in Caries Research, a finding that has not been formally disputed in the peer-reviewed literature.
That part is real. I used to assume the whole fluoride-pineal connection was conspiracy noise until I actually read the study. Then I read the methods. And that’s when it got complicated.
Eleven cadavers. Average age of 82. From one geographic region in the UK. No control group of fluoride-unexposed individuals. And critically — no measurement of whether those concentrations impaired anything the gland was actually supposed to do.
Accumulation is not damage. Hold that distinction. Everything downstream depends on it.
Yes — in animals, at doses nobody in the US is consuming from tap water.
Luke’s 1997 dissertation showed gerbils exposed to fluoride had measurably lower nighttime melatonin and earlier puberty onset compared to controls. A 2014 study in the Fluoride journal by Bhattacharya and colleagues found similar results in rats — reduced nocturnal melatonin synthesis, histological changes in the pineal, fluoride concentrations correlating with measurable disruption.
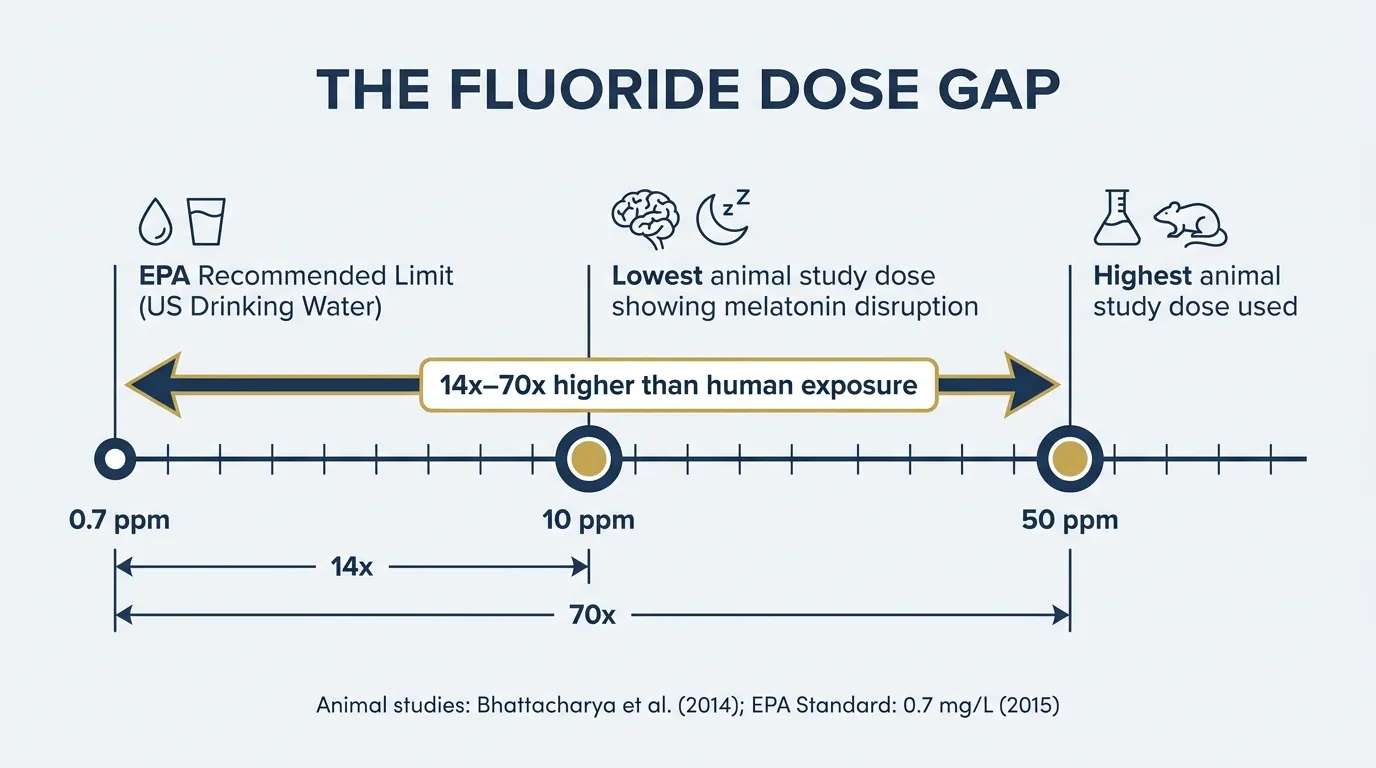
The doses used? Between 10 and 50 parts per million in drinking water. The EPA’s current recommended maximum for US drinking water is 0.7 mg/L — 0.7 ppm. The studies showing measurable effects used concentrations 14 to 70 times higher.
That’s not a small gap.
I’m not saying it makes the concern irrelevant. Animal data on mechanisms is worth taking seriously — especially when the mechanism is plausible and the target tissue is confirmed to accumulate the compound in question. But if the threshold requires exposure an order of magnitude above what most Americans consume, the public health extrapolation needs a lot more support than it currently has.
If you’re the kind of person who’s already switched to filtered water, questioned your fluoridated toothpaste, and started asking questions your dentist looks uncomfortable answering — you’ve probably felt the frustration of not getting a straight answer from either side. That frustration is legitimate. The gap in human research is real, and it’s been real for 25 years.
Here’s what’s actually happening when we talk about pineal calcification: it’s extremely common, it begins early, and fluoride is almost certainly not the primary driver.
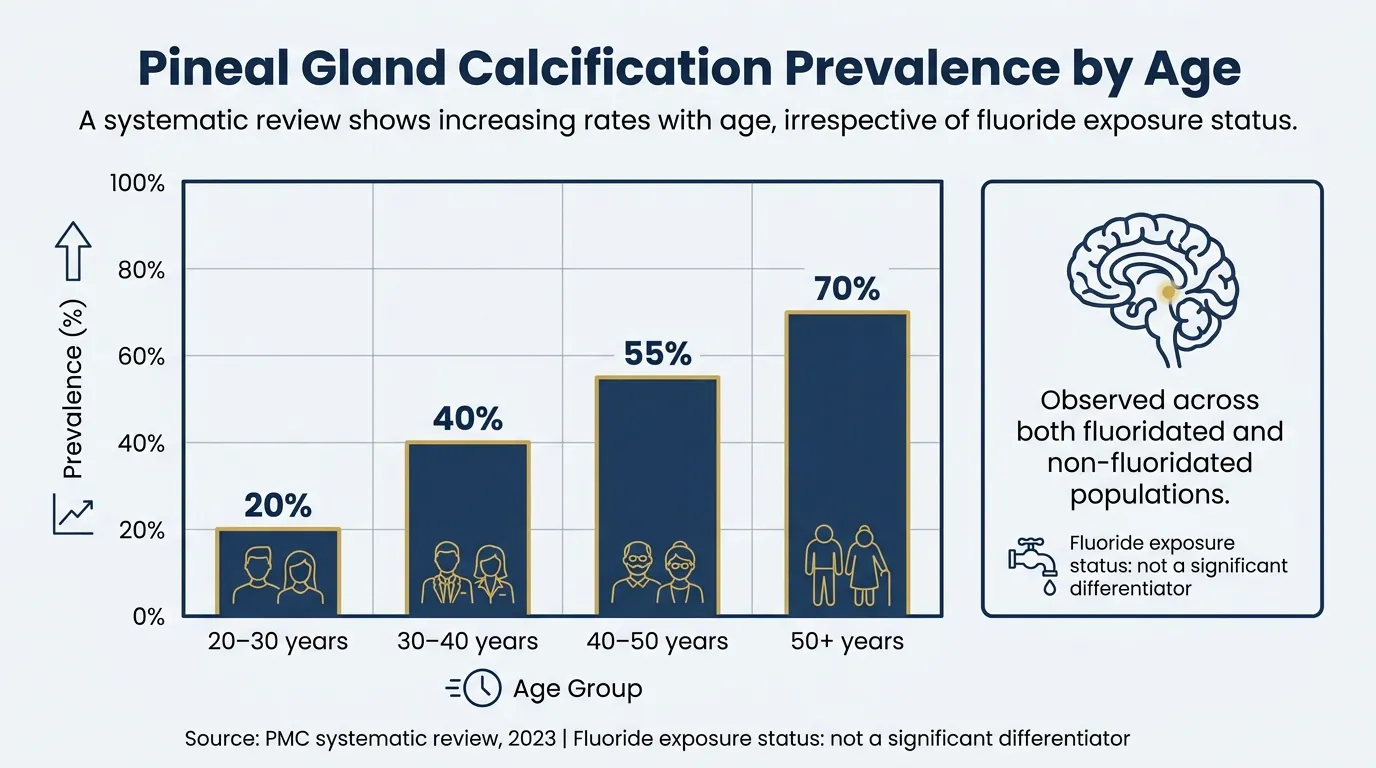
Multiple neuroimaging studies — including data from a 2023 systematic review published in PMC — show pineal calcification is detectable in 50 to 70% of adults on standard CT scans, and prevalence increases with age across populations regardless of water fluoridation status. A Brazilian cohort study documented physiological pineal calcification in up to 70% of patients reviewed.
That complicates the narrative considerably.
If fluoride were the primary cause of pineal calcification, you’d expect populations with lower fluoride exposure — non-fluoridated water regions, low-fluoride countries — to show meaningfully lower calcification rates. The imaging data doesn’t consistently support that. Calcification appears to be a function of aging, calcium metabolism, and probably genetics. Fluoride may accelerate or worsen the process rather than initiate it.
That’s a meaningful distinction. Nobody in either camp wants to make it, because it doesn’t serve a clean story.
And here’s the question that genuinely unsettles me: if the pineal gland calcifies in the majority of adults by their 50s through mechanisms that predate industrial fluoridation — what does that say about its function in most people walking around right now? That’s not an argument for ignoring fluoride. It’s an argument for taking calcification itself more seriously, regardless of the cause.
The most important things about fluoride pineal gland calcification research are the things it cannot answer yet.
No published longitudinal human study has tracked fluoride exposure against pineal function or melatonin output over time. None. The closest we have are cadaveric tissue studies — dead tissue, limited samples — and animal models using doses that don’t match human exposure.
There’s no established dose-response curve in humans. Nobody has mapped the relationship between real-world fluoride intake from water, toothpaste, and food against measurable changes in nighttime melatonin in living people.
Reversibility. Nobody has studied it. Switch to filtered water and low-fluoride dental products for five years — does your melatonin improve? Does your pineal look different on imaging? Genuinely unknown. We’ve reviewed what reversal protocols do have evidence behind them — fluoride reduction isn’t among the studied interventions, though it remains a logical precautionary step.
I’ve had experiences I can’t explain with a PubMed search. But I won’t tell you the published data supports conclusions it doesn’t reach. Here’s where the evidence actually stops: we know fluoride accumulates in the gland at high concentrations in aged tissue. We have animal data suggesting functional consequences at supraphysiological doses. We have no controlled human data on function, threshold, or reversibility.
That’s the gray zone. Not disproven. Not proven. Genuinely unresolved — and that unresolvedness has persisted for 25 years not because the question is unanswerable, but because almost no one is trying to answer it.
The absence of research is not evidence of safety. It’s evidence of a funding gap that should bother you regardless of where you land on the fluoride debate.
Here’s where diet and lifestyle hit a ceiling for most people. You can filter your water, cut fluoridated toothpaste, and reduce dietary sources — all sensible moves. For a more comprehensive approach to reducing pineal burden, a structured detox protocol is a reasonable next step once the basics are covered.
Start with the water filter. It’s the highest-exposure vector, it’s addressable today, and if the human evidence eventually catches up to the animal data, consistent reduction in the highest-volume input is where you’d expect to see any signal first. Reverse osmosis removes fluoride effectively. Most pitcher filters don’t — check the specs before assuming.
After that, sleep hygiene matters more than any supplement. The pineal gland’s melatonin output responds to light exposure, sleep timing, and circadian consistency before it responds to anything you swallow. Get those right first.
Then, if you want to look at formulated support, the stack worth examining is iodine and magnesium — two nutrients with documented roles in pineal enzyme activity and melatonin synthesis. Look at the label, check the doses against the actual literature, and be skeptical of anything claiming to “open” anything.
Pineal Guardian is the one product in this space that doesn’t embarrass itself on the label — the iodine, magnesium, and antioxidant stack reflects the mechanisms in the animal literature rather than just listing popular ingredients in a “proprietary blend.” That’s a low bar. It’s also one most products in this space can’t clear.

Quick Verdict — Pineal Guardian

A liquid botanical formula targeting pineal support via iodine, magnesium, and an antioxidant stack. Ingredient selection reflects the mechanisms identified in the fluoride-pineal animal literature rather than generic 'detox' marketing. 365-day guarantee.
Compare the clinical doses of each ingredient before deciding.
Disclosure: This article contains affiliate links. If you purchase through these links, I may earn a commission at no extra cost to you.
Marcus Hale is an independent researcher and former clinical neuroscientist. The content on PinealCode.com is for informational purposes only and does not constitute medical advice.

10 pineal gland supplements ranked by evidence score — not marketing claims. Magnesium scored 8.4/10. Most popular products ranked lower...
61.65% of adults have pineal calcification — and the internet promises a 30-day fix. Actual research timeline: 3–6 months. Week-by-week...
Can pineal gland calcification be reversed? Yes — with important caveats. See what the research shows, what works, and realistic timelines.

Marcus Hale
Independent Researcher · Former Clinical Neuroscientist
I spent 12 years in clinical neurology before the questions got more interesting than the answers. PinealCode is where I document what I find at the intersection of brain science and consciousness.